Seborrhoeic dermatitis has been the bane of my skin for a long time. In my case, I was first officially diagnosed at around age 20, but in all likelihood it’s been contributing to my skin woes for quite a while.
It’s finally time that I present to you: my complete guide to seborrhoeic dermatitis identification, treatment and management. I wanted to put all the information in one place and strip it down to the need-to-knows, with actionable suggestions based on my personal experience as well as research I’ve gathered on the topic.
Seborrhoeic dermatitis is a skin rash. ‘Dermatitis’ means a problem with the skin. This indicates it’s loosely related to contact dermatitis (allergy) or atopic dermatitis (eczema). Seborrhoeic (also spelled seborrheic) means ‘related to sebum’. So, seborrhoeic dermatitis is a rash-like skin condition that appears in areas of high concentration of oil glands.
Chronic skin conditions like seb derm are tiring, demotivating and uncomfortable. But if you’re struggling with seborrhoeic dermatitis, you’re not alone.
Features and symptoms: What does seb derm look like?
So, want to know whether your rash could be seborrhoeic dermatitis. With so many different kinds, it can be tricky to narrow down what kind of rash you’re dealing with. Luckily, seb derm has a reasonably distinct set of characteristics that set it apart from many other conditions.
Seb derm comes with:
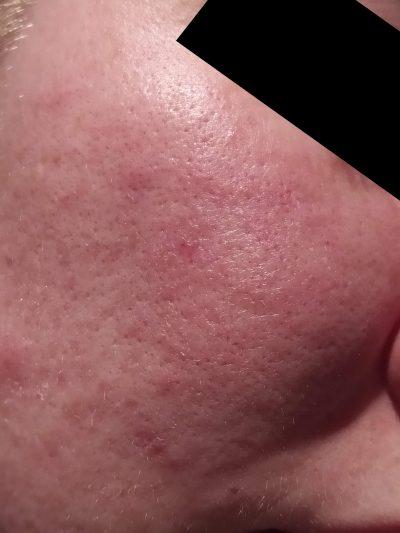
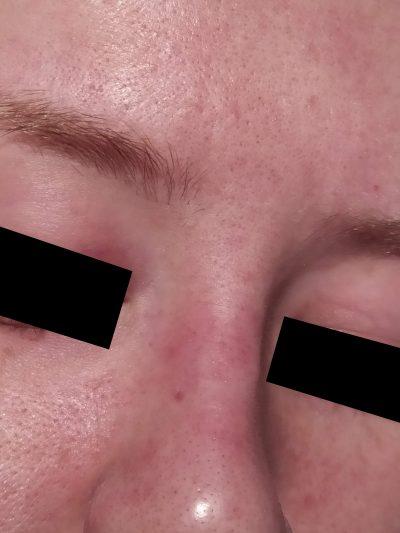
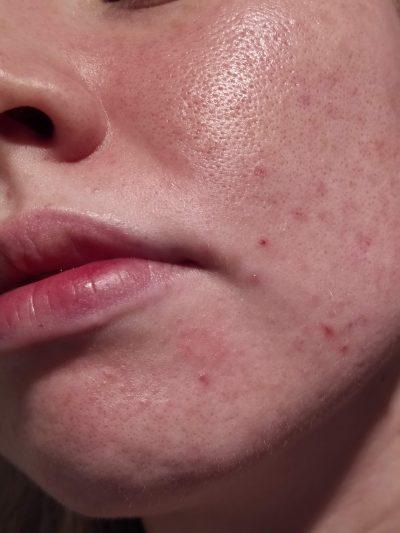
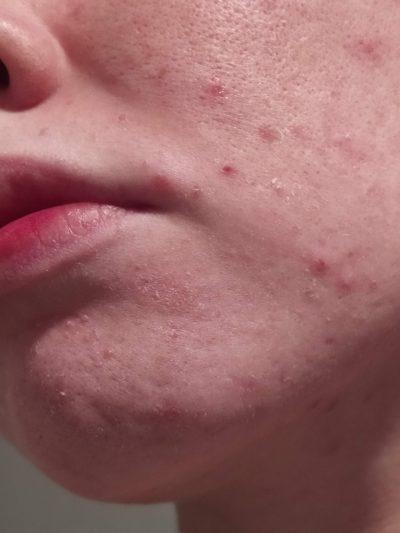
- patchy facial redness
- patchy hypopigmentation (lightening of the skin colour) in darker skin tones
- raised, dry-looking or greasy plaques
- small stubborn flakes
- itching
- papules (raised, red bumps without pus or openings)
- exclusively facial, ear, neck, scalp and chest presentation
- a recurrence pattern that flares and wanes
What causes seb derm?
The strange and unique features of seb derm make more sense once you start to learn why it happens. There are two parts to understand: the ‘mechanism of action’ or why your skin is acting the way it is, and why it’s happening specifically to you/who is most susceptible.
What happens inside the skin?
Seborrheic dermatitis at its core is an Inflammatory condition which most dermatologists agree is caused by an allergic/sensitivity to unsaturated fatty acids produced by potentially excess naturally yeasts from the skin, Malassezia, when they metabolise sebum.
You see, when you have oily skin, there’s lots of great food for natural fungi to feed on. And the more oil, the more those yeasts thrive. When Malassezia eat your sebum and turn it into energy for themselves, they break it down into smaller components, specifically unsaturated fatty acids. This is left behind on your skin surface, and once it works its way amongst your skin cells can then impact the health of your skin barrier. This leads to the itchiness, redness and scaly flaky skin typical of seb derm.
Seb derm is considered to be either an overabundance or oversensitivity to the Malassezia yeast and their presence. It’s a vicious cycle where more oil = more yeast = weakened skin barrier = more yeast and so on.
Who gets seb derm? Why do I have seb derm?
Seb derm is one of the most common skin diseases. That’s good news for you though, because it means there’s been a lot of research into its genetic and environmental causes, as well as treatments. So don’t feel alone!
The main risk factor for seb derm is having oily skin. It also tends to get out of hand in people with suppressed immune systems. Genetics patterns have been found in developing seb derm, but specific genes are still being identified.
It’s also important to know that seborrhoeic dermatitis is related to, if not the same as, cradle cap in infants (which I apparently suffered from) as well as dandruff (which my sister suffers from). So if you dealt or deal with either of those issues, or those in your family have them or seb derm, that increases your likelihood of having it too, and the treatments are very similar.
What are the treatment options for seb derm?
Treating seb derm holistically requires a three-pronged approach – managing the fungi, inflammation, and flaking/scaling.
Reducing fungal colonisation
Because fungi are at the top of the suspect list for seb derm triggers, even though they’re harmless on a lot of people’s skin, you definitely want to focus on reducing their presence. You’ll never eliminate them totally because it’s not an infection, but you can reduce the load they’re putting on your overacting immune system.
Antifungal cream
Ketoconazole is the most well-known treatment for seb derm. If that doesn’t work, miconazole, terbinafine, or any number of other antifungal agents are effective. It often takes trial and error to find one that works best for you.
Antifungal shampoo
The shampoo works in much the same way as the cream, but it’s soemtimes thought to be easier to apply, especially to handle seb derm in the hairline and behind the ears, or as a preventative or maintenance treatment. You apply like a cream and allow to sit on the skin before getting in the shower and lathering and rinsing a few minutes later. Ketoconazole, selenium sulfide, and zinc pyrithione are just some of the active ingredients that you can find in these products.
Reducing inflammation
A major key in the seb derm puzzle is realising that your skin is overreacting (drama queen…). Inflammation is the middle man between the fungal cause and the visible symptoms, but it’s also the thing that’s hardest to treat because it’s such a core part of our body’s natural systems. Especially when it comes to managing flares, but also to a lesser extent in the every day products you choose, the focus should be on calming and inflammation-reducing.
Steroid cream
This treatment offers the most immediate, impactful improvement in seb derm. It works by temporarily turning off your skin’s inflammation response. It’s unbeatable in terms of getting on top of an outbreak and giving your skin a chance to heal. Unfortunately, it’s only a temporary solution for acute flares, not something long-term. It should be used sparingly and for short bursts at a time – never longer than a few weeks, as this can lead to long-term steroid dependencies which cause much worse rebound problems.
Soothing ingredients
Things like allantoin, bisabolol, and green tea are among many calming ingredients that help to relieve itching and irritation, and they can be used as often as you want. Find products containing these ingredients and more in my anti-redness recommendations.
Removing scaling
This is an option that’s just treating the symptoms, not the cause, but it will improve the look of the rash as well as the extra benefit of allowing your other topical products to work better, because they don’t have to fight so hard to get through to your skin underneath the hardened dry surface. Using the below products regularly will help to keep your flaking and scaling under control.
Gentle AHA exfoliants
These help to loosen the bonds that keep dead, dry skin stuck together on the surface and encourages it to slough off instead. I lean towards mandelic acid because it’s super gentle and supposedly good for acne sufferers. Other popular and slightly stronger AHAs include lactic and glycolic acid.
Urea
Urea is fantastic because not only is it a gentle keratolytic (dissolving agent) like AHA, but it’s also a powerful humectant. That makes it doubly effective in reducing scaling, because it also hydrates the flakes and makes them appear better temporarily.
Sulfur
Sulfur is an old-school treatment for just about any skin issue. While it doesn’t smell the best, it’s antifungal (good for fighting those yeast), antibacterial (good for lingering acne) and keratolytic.
Further recommended lifestyle changes
Aside from what’s in your skin care routine to teat your seb derm, there are some other habits you can make which will have a positive effect on how your seb derm looks and how often it flares.
Reduce oil
Excess oil is a predisposing factor to seb derm because it feeds the yeast, encouraging them to thrive and gives them more fuel to turn into irritating unsaturated fatty acids. Whatever you can do to manage oil production will help. That means washing your face frequently (two times a day is plenty), use a product like niacinamide which can balance excess sebum production, check your hormone levels with a doctor, and in extreme cases consider treatment with isotretinoin, which will permanently reduce your sebum levels.
Increase sun exposure
I know, this doesn’t sound like me. Usually I’m encouraging you to cover up and slather on sunscreen. But the yeast that trigger seb derm really don’t like UV exposure. Many people can back this up anecdotally, saying that going to the beach or on holiday really clears their skin. So within reason, give yourself a little bit of sunlight on your face daily.
Reduce stress
Ugh – I know, it’s a vague suggestion. But basically anything that puts your body, mind or skin in a position where it’s not being looked after properly can trigger seb derm. So fixing that means cutting out your worst habits and putting energy into your mental health – bonus, even if your skin doesn’t get better, you’ll be healthier and happier overall.
What should you avoid?
High oil/saturated fatty acid content ingredients
This is like fungi’s ideal dinner. They chomp on those oils and make metabolites which are what causes your scabby, red skin in the first place. So giving them more food = giving them the ammunition to make your problems worse. Stay away from things like natural plant oils and butters!
Scratching
Scratching releases histamine, which causes more swelling and redness. It also spreads oil , fungus and bacteria. And of coursek, it removed skin cells and leaves superficial skin damage which is just more opoprtunity for infection.
Scrubbing
Just don’t do it! Those little flakes will come right back; they’re there because your skin barrier and epidermis is highly irritated. You need to treat the source of the problem, and scrubbing the flakes off will just make them worse the next day.
Natural remedies
Because seb derm is such a prolific and damaging disease, there’s naturally a ton of discussion and support on online forums. That makes it easy to find people to talk to and get recommendations from, but can make it hard to focus on the most effective treatments. People are always giving anecdotal advice for what works for them, and just through selection bias the people who flock online are those for whom conventional treatments don’t work as well.
I’m absolutely not saying that these remedies don’t have the potential to work, it’s just often tempting to skip over medications and doctors and go straight to these first, which can often actually cause undue stress and wasted time. I would recommend trying the aforementioned conventional treatments first, before trying out things like raw honey masks.
My advice for what to expect through treatment and in the future
Here’s my current daily anti-seb derm routine for you to base yours on:
- CeraVe SA Cleanser
- Terbinafine cream
- Urea and lactic acid moisturiser OR CeraVe Moisturising Cream
- AM only: Sunscreen
- Steroid cream as needed
Typically, studies for various treatments look for results at 4 weeks and 8 weeks, and sometimes do a check up at 12 weeks. This is because even when you’re doing the right thing, it takes a long time for your skin to heal from the damage and start to look normal again. I’ve been dealing with a bad flare for over a month now.
If you notice improvement in the first week and then plateauing or worsening, it’s probably that you’re using the right approach (anti-fungal treatment) but you need a different anti-fungal.
Seborrhoeic dermatitis is not something you can really cure. It’s a predisposition. You can remove all the symptoms but in all likelihood when you stop treating the issue it will eventually come back. Seb derm treatment is something you’ll probably need to incorporate forever.
My advice: stop reading about seb derm and your skin after this. It’s so easy to want to assume your skin has all sorts of problems it doesnt, or to read and read and read in hopes you’ll read something new and easier. But in reality, it’s the day-to-day approach that works best. Don’t wear out your mental muscles.